It’s the first time in MONTHS that I’ve been up in the middle of the night…I guess I should be thankful for that! But tonight/this morning, I find myself awake and pumping while Struthers sleeps soundly so I might as well use the time to update you on a lot that has transpired over the last week!
We had four specialist appointments over three days last week, and getting to each of those on time and in one piece, while not missing a beat with work was quite the accomplishment! We are getting used to the oxygen and being ‘out’ a bit more, with a newfound respect for all our friends with multiples–HOW do they do it?!?! I’m just now mastering new-parent skills like changing diapers on the go, feeding in the backseat of the car (parked of course!), pumping on-the-go, walking into an appointment or church with just the bare minimum of a diaper, wipes and feeding tube in my purse instead of hauling in the loaded down diaper bag…after all, there’s enough ATTACHED to him, WHY would we carry any more than we have to?!?
So here’s the rundown of each appointment:
- Surgical followup with Dr. Shipman: His G-button site looks better after now two silver nitrate treatments. The silver nitrate just helps the raw edge of the skin around the tube kind of scab up instead of produce more skin cells (granulation tissue) that our body naturally does in order to close/heal any wound. The button itself is a piece of plastic that sticks through the skin, so until it is out, you want to prevent the body from doing its natural ‘close this up’ thing. We change his dressing site daily, and I alternate using disposable split gauze pads and these cute little fabric ones with elephants, frogs and chevrons I found on Etsy (they’re much more absorbent). We are still using the tube for about 2-3 feedings per week, really only when Struthers conks out early and just needs the additional calories for the day. We use it mostly to vent and allow air and stomach acid to escape…things babies can normally do through burps or spitup, unless they’ve had a Nissen that keeps things from coming back up. The tube will likely be in place for another 6 months or so, but once we get to the point that it’s not being used at all over a few weeks, it will be removed. For now, Struthers doesn’t even seem to notice it, except that he kind of plays with it and spins it around as he’s discovering his hands…I guess that answers my question about whether it pulls or hurts him! Just to clarify, there are multiple types of infant feeding tubes. There are NG tubes which go through the nose (you may remember the orange line in all of Struthers’ NICU photos) and OG tubes are the same little orange ones through the mouth (he had this one during the NICU months he was on CPAP). Both of these types are for more temporary enteral feedings, and the tubing can just be pulled in and out and is generally changed weekly. A G-button, however, is a more long-term feeding solution that is actually surgically inserted under his skin, much like a port. While I fought and put this off (for way too long), it’s turned out to be the very best thing and we are overjoyed at the growth Struthers is experiencing with it!
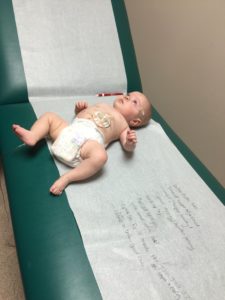
- GI Followup with Dr. Barrios: Struthers in GROWING!!! He’s now 12 pounds, 9 ounces and 24.5 inches long! At 7.5 months, this still places him well below his growth curve for his actual age. But he’s now in the bottom 2nd percentile of that growth curve based on his adjusted (due date) age of 4.5 months! He’s not doing the massive catchup growth jumps they’d like to see, but he’s plodding along on his own little curve still. So what now? We will continue to fortify his breastmilk bottle feeds to 24-calories (normal breastmilk is @ 20 calories). And though he’s been on rice cereal since the week we brought him home, we are now venturing into solids at the encouragement of Dr. Barrios. We tried mushed avocado last night, and I’m not sure a single bit actually made it down his throat! I’m questioning whether he’s actually ready, as he didn’t seem to know how to swallow the puree and then choked a bit, scaring me half to death. But we will keep trying with the help of his therapist this week, as I understand that even with a preemie, it’s important to introduce him over the next few weeks. But I also don’t want to force the issue and contribute to any oral aversions.
- Urology consult with Dr. Blythe: It has been debated since shortly after his birth whether the swelling and fluid in Struthers’ groin area was a hydrocele or inguinal hernia. Long story short: we’re still not sure. So there are two types of hydroceles: non-communicating and communicating. Non-communicating ones will eventually go away on their own as the body absorbs the extra fluid. Communicating ones are where the fluid travels freely back and forth from inside the abdominal cavity, and they require surgical intervention prior to a closing up of the area (hernia) that could leave tissue without blood flow. So we will follow up with Dr. Blythe in about three more months, and I’ll watch for whether the swelling fluctuates or is constant, with perhaps slight decreases.
- Pulmonology followup with Dr. Guarin: He’s doing OK, with steady improvement! The main factor for preemies being able to outgrow their chronic lung disease is whether they are growing and putting on weight. So on that front, we are doing OK, but need to continue doing all the extra things outlined by Dr. Barrios to keep that moving along. Respiratory issues and growth are such a catch-22 because one can’t happen without the other. So our pulmonologist put it this way as she wrote out a script for another maintenance steroid, “If he’s working hard to breathe, he won’t be able to grow. If he can’t grow, he’s not growing new lung tissue to help him breathe easier. So I’m going to do everything I can to help him not work hard with these medicines. Then hopefully, he can grow and will outgrow the breathing issues.” OK-that vicious cycle seems simple enough. So Struthers still visibly retracts when he breathes, which is when the skin pulls in and out between each rib, indicating difficulty breathing. Our little fighter manages to keep his oxygen saturation above 90, but his little body is working fairly hard to do so. What does that mean? We will keep his oxygen levels where they are now (1/8 liter during wake time and 1/4 liter during sleep). I kept hoping we would be able to wean down by now, but he’s just not ready, so I’m learning a healthy dose of patience. And given the process for weaning and followup intervals/timing, I think we’ll be lucky to be off daytime oxygen by his first birthday. And we could be on nighttime for years, until he outgrows the apnea. Sigh. But if it helps him, I’m all for continuing to play jump rope with tubing throughout the house and car.

NICU visit while we were in Denver: We coordinated one of our Denver appointments with the opportunity to swing into the University NICU at the same time as our former NICU neighbors, the Mentel triplets (and parents) made a visit back. It was amazing to see these precious girls and their parents and Babcia (Polish for grandma). The most amazing part was the grace and ease with which Marta handled THREE girls simultaneously AND was so intently trying to catch up on how we were! Gabi, Skyler and Harper are beautiful and growing, and we look forward to years of staying in touch with them!
Again, THANK YOU for the prayers and love!
Eli, Cami and Struthers
Comments imported from CaringBridge (6 comments):
Love hearing your progress reports. Love that he is growing and making progress. Praying that it just gets better and better.
—Lisa Lindley, June 29, 2015
Thanks for your informative update.Might want to try applesauce that would taste better. Hugs for you all.
—Marj, June 29, 2015
Many thanks for the detailed and very informative updates Cami. We continue to hold you, Struthers, and Eli close in our hearts, thoughts and prayers! Love and Special Blessings ….
—Rick and Billie Broome and Family, June 29, 2015
Thanks for the update Cami. Even I don’t fully understand what is going on sometimes, I always enjoy reading your posts. Y’all are still in our thoughts and prayers. Love y’all.
—David Summerall, June 29, 2015
Thanks for the update, Cami. Prayers for all three of you!
—Ann Alvis, June 29, 2015
Praying for this little guy everyday! God Bless you all! Hugs! ??
—Milli Sample, June 29, 2015